The ALL: 10 facts about this outer ligament
An ALL reconstruction, LET or Lemaire plastic. Three different names for the same thing - a procedure to restore rotational stability to the knee. This is an important function of the ALL and in this blog you will read all about this particular ligament.
The discovery of a new ligament the ALL
We thought we knew everything about the knee, but in 2013, under the watchful eye of the international press, news emerged from Belgium. Two researchers discovered a new ligament on the outside of the knee. It is called the Anterolateral Ligament, abbreviated as the ALL. "Anterolateral" refers to the front side, and "lateral" refers to the outside, indicating the location of this newly discovered ligament.
Michael de Levie and Aernout Zuiderbaan Orthopedic surgeon at the Medische Kliniek Velsen.
Is the treatment of the ALL new?
Over 50 years ago, a torn anterior cruciate ligament was already a well-known and notorious knee injury. Back then, anterior cruciate ligament reconstruction was performed using the popular Jones technique. The cruciate ligament was replaced with a body's own tendon central to the knee. However, the surgery did not always result in a stable knee. It frequently occurred that the knee remained unstable during rotational movements. This regularly led to a re-rupture. We call the instability anterior lateral knee instability or anterolateral angle instability.
From the French side, a solution emerged to stabilize rotation. The operation was named the Lemaire plasty, named after an orthopedic surgeon from Lyon. It was the precursor to the current ALL reconstruction. Interestingly, at that time, nothing was known about that ligament (ALL), but the vision of how to restore stability was ahead of its time. However, the surgical techniques of that era were not up to today's standards. The Lemaire plasty was a major operation with a large incision, which increased the risk of infection. Over the years, surgical techniques have improved, and by anatomically placing the anterior cruciate ligament, the problem of rotatory instability was partially solved. The Lemaire plasty faded into obscurity.
The knee remains unstable
Although modern anterior cruciate ligament reconstruction is a successful surgery, a proportion of operated patients still continue to experience instability complaints. On physical examination, the knee is unstable in rotational movements, while the knee is stable in forward movements. Thus, forward, backward stability is restored (Lachman test). Due to rotational instability, a number of patients are not satisfied with the outcome of surgery. They continue to experience instability, mainly in high impact sports and sports with a lot of turning and turning (soccer, field hockey, rugby etc). For this group of patients, sports resumption is not possible or adapted as the risk of re-rupture is increased. The discovery of the ALL and its treatment may possibly provide the solution.
What is the ALL?
It is a small band or reinforcement of the capsule on the outside of the knee (see photo). It runs from the femur to the Gerdy's tubercle. Due to its position, this ligament has a significant influence on stabilizing rotation. The anterolateral ligament (ALL) is believed to have an even greater stabilizing function in rotation than the posterior bundle of the anterior cruciate ligament (one of the two bundles of the ACL).
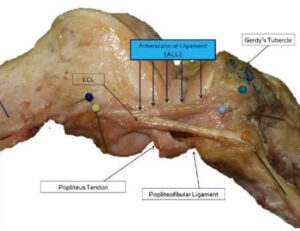
How do you know if the ALL is torn?
If you have a Segond fracture (see photo), you have a 100 percent chance of a torn anterior cruciate ligament (ACL), and it is likely that the anterolateral ligament (ALL) is also damaged. A Segond fracture is an avulsion fracture where the attachment of the ALL is pulled off the bone. If a Segond fracture is not visible on the X-ray, the ALL can still be torn. A reasonably accurate diagnosis can be made through physical examination. A torn ALL is difficult to visualize on an MRI scan. The ALL can be well assessed during surgery. For the surgeon, this is the optimal moment to reevaluate the knee before performing the ACL reconstruction. It is not uncommon for the orthopedic surgeon to decide during the operation whether an ALL reconstruction is necessary.
Examining a ruptured ALL
Forward mobility (Lachman +), rotationally stable (Pivot -) → no ALL
Forward mobility (Lachman +), rotationally stable (Pivot -/+) → no ALL
Forward mobility (Lachman +), rotationally unstable (Pivot +) → ALL
(- = negative, -/+ = doubt, + positive)
A positive pivot shift is a good indication to do an ALL reconstruction in addition to an anterior cruciate ligament reconstruction. However, there are other situations to do an ALL reconstruction. More on this later.
The ALL procedure
There are several surgical techniques to reconstruct the anterolateral ligament (ALL) or reinforce the outer part of the knee. The Lemaire plasty is a technique where a strip is taken from the iliotibial tract. This strip is passed beneath the lateral collateral ligament (outer band) and fixed to the femur bone. This creates a connection between the tibia and femur, preventing internal rotation of the tibia. This technique is also referred to as lateral extra-articular tenodesis (LET).
Click here For a video about the LET surgery performed by Dr. R. Hoogeslag from OCON in Hengelo.
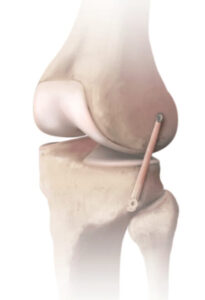
The other technique is an ALL reconstruction. The ALL reconstruction is a technique where a tendon or artificial ligament is used and secured with a screw in the femur and a screw in the tibia. Typically, the gracilis tendon is used for this procedure.
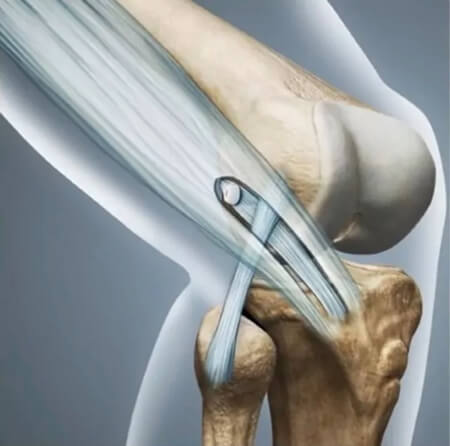
Who is eligible for treatment of ALL?
Patients who are at increased risk of or have re-torn their anterior cruciate ligament reconstruction are eligible for treatment of the ALL. Hypermobility, hyperextension of the knee (space overstretching) and a positive pivot shift test causing rotational instability of the knee are reasons to perform an ALL reconstruction, LET or Lemaire procedure. The physician, as mentioned above, can assess this well. In high-risk sports, the physician may decide to add an ALL as a precaution. After a re-rupture, an ALL reconstruction, LET or Lemaire plastic is almost always used in addition to an anterior cruciate ligament reconstruction.
What does physical therapy look like after an ALL procedure?
Post-treatment varies by physician. The doctor may choose to provide an extension lock brace. (foto brace) The brace can be adjusted to flex up to 70 degrees in the first two weeks after anterior cruciate ligament reconstruction. After two weeks, the brace is adjusted to 90 degrees of flexion. After six weeks, the brace is tapered off. A second option is to wear an extension lock brace for six weeks that is adjusted to 90 degrees of flexion. The third and most common post-treatment option is no brace. The knee may be flexed based on pain and after reaction.
Most patients have more pain initially after an ALL reconstruction, LET or Lemaire plastic procedure. This is due to the 8- to 10-centimeter skin incision that is on the moving part of the knee. The patients with a brace, complain more often of knee stiffness. Thereby, a brace usually results in a disturbed gait pattern. As a result, regaining a symmetrical gait pattern takes longer. Another inconvenience is that the brace often slips off. Recently, new braces have come on the market that are more comfortable to wear. Furthermore, rehabilitation after an ALL procedure follows the protocol of an anterior cruciate ligament reconstruction without ALL.
The ALL combined with anterior cruciate ligament reconstruction.
Since the addition of ALL reconstruction to the orthopedic surgeon's repertoire, there has been a clear decrease in the number of re-ruptures. The outlook is promising, although it is still somewhat uncertain how the long-term effects will be in relation to osteoarthritis and other knee complaints.
or click here For a video about the LET surgery performed by Dr. R. Hoogeslag from OCON in Hengelo.
Indication:
Not everyone needs this surgery and is especially recommended for patients at high risk of rupturing their anterior cruciate ligament again;
- Patients with hyperlaxity/hypermobility
- Patients under 30 years of age
- Revisions of a previously performed anterior cruciate ligament reconstruction
- Topsporters die kap- en draaisporten beoefenen zoals voetbal, hockey, tennis en handbal
Is there scientific evidence for the treatment of the ALL
Recent well-conducted scientific research shows that ALL reconstruction reduces the risk of re-rupture of the anterior cruciate ligament in young patients who have undergone ACL reconstruction. The percentage of re-ruptures of the ACL reconstruction decreased by 70%, from 11% to 4%.
Summary
experienced orthopedic surgeon who can assess your specific condition and determine whether an ALL reconstruction is necessary. The decision should be based on a thorough evaluation of various factors, including your age, activity level, injury history, and individual needs. Seeking expert advice and personalized recommendations will help ensure the best course of treatment for your specific case. knee specialist How the long-term effects will be will remain to be seen, but as mentioned, the outlook is good.
This blog was created in collaboration with Aernout Zuiderbaan orthopedic surgeon in the Velsen Medical Clinic
Related Articles
Related
Tips for finding a knee specialist (physio)
Tips om een kniespecialist (fysio) te vinden Het resultaat van een knieoperatie (voorste kruisband reconstructie) valt of staat met een goede revalidatie. Verschillende factoren beïnvloeden de revalidatie, waaronder ziekte, reizen en andere verplichtingen. Ook de...
What is an ALL reconstruction or Lemaire plastic (LET)?
Wat is een ALL reconstructie of Lemaire plastiek (LET)? Doe jij een risicovolle sport (voetbal, basketbal, etc), dan krijg je naast een voorste kruisband reconstructie waarschijnlijk ook een extra versteviging aan de buitenzijde van de knie (ALL). Op de verwijzing...
Why does anterior cruciate ligament rehabilitation take so long?
[lwp_divi_breadcrumbs _builder_version="4.22.2" _module_preset="default" global_colors_info="{}"][/lwp_divi_breadcrumbs]Een voorste kruisband revalidatie duurt gemiddeld 9 tot 12 maanden en soms langer. Na de revalidatie verwacht meer dan 90 procent van de...