Dummy
Meniscus surgery and treatment
Information about knee keyhole surgery and the various treatment options for a torn meniscus.
Conservative:
Preoperative
Operative:
Rehab
Result
Risk
Cost
Recovering without surgery after a torn meniscus.
One of the main functions of the meniscus is to protect the articular cartilage. If the meniscus is torn, you can choose a conservative or surgical course. Research shows that the risk of knee osteoarthritis increases after meniscus surgery (meniscusectomy). Therefore, the goal is to preserve the meniscus and the goal is to recover conservatively. The choice of conservative repair has been shown by research to be proven effective. This is mainly true for the degenerative meniscus tear (>45 years and older). Nevertheless, rehabilitation without surgery is also intended for younger people (<45 years of age). A locked knee (knee can no longer bend or extend) is a hard indication for surgery. If you have trained specifically and continue to have symptoms, surgery is also possible (applies especially to the <45 year old group). As a rule, elite athletes usually undergo surgery. Discuss with your doctor what is the best treatment for you.
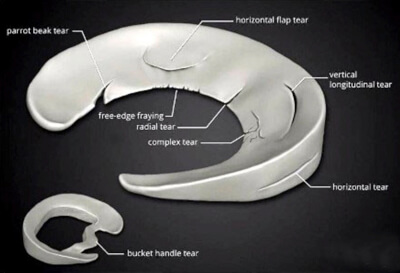
Various tears of the meniscus
A conservative trajectory:
Most people have overused their knee due to a long walk, sports strain or sports injury. Sometimes the symptoms are variable and/or prolonged. Minor to moderate swelling is usually present and bending and/or stretching is stiff. Muscle strength has decreased and may feel and/or be unstable.
The focus of treatment is to re-optimize mobility (bending/stretching) and strengthen the leg muscles. Try regular cycling (exercise bike) and take a bike rather than a walk. In addition to strength, doing stability and coordination exercises is a good complement to recovery.
Living rule advice:
- Cycle regularly
- Try not to walk or stand for too long at a time.
- Take care when bending over (avoid deep squatting at first and bend the knee to a maximum of 90 degrees)
- Be careful with rotational movements
- Stop exercising temporarily, but seek an alternative in consultation with the doctor or physical therapist.
- Get advice regarding load management.
- Weight reduction may be optional.
Once the pain has subsided, the load of exercises can be gradually built up. Stretching and bending of the knee improves and deeper knee bends are possible again. As much as possible, the exercises should be functional combined with targeted strength exercises. Get advice from a physical therapist for this.
Especially for athletes, in addition to leg exercises, do exercises to support the entire movement chain (trunk, hip, back, etc).
If the recovery is successful, then the load can be further increased. Here the different and personal goals determine the direction of rehabilitation.
Advice:
During recovery, especially in the beginning, it is not bad to have intermittent symptoms. The load capacity of the knee is still low and the knee can quickly become irritated. Be patient and at least 6 to 12 weeks of recovery is necessary to speak of a successful or unsuccessful rehabilitation.
Preoperative training: better in, better out.
In the past, a meniscus was removed immediately when there were complaints. Today, we know that the meniscus provides stability and protects the underlying cartilage.
Except in elite sports and subtop, meniscus surgery in recreational sports is not necessarily the first choice. Provided you have no lock symptoms, a conservative course (no surgery) is preferred.
Strengthening the thigh muscles, exercising the entire movement chain and optimizing stability and coordination has been shown by multiple studies to be a good treatment. Should insufficient effect still be achieved after a course of physical therapy, you did not train for nothing. The saying "better in, better out" applies here.
Why preoperative exercise helps:A meniscus problem causes an inflammatory reaction in the knee. The result is swelling. Fluid in the knee negatively affects the upper leg muscles, stability and coordination. Another problem that can occur is a stiff knee when bending and stretching. Good knee function before surgery is a positive indicator of your recovery after surgery.
A preoperative course consists of an informational interview in addition to muscle training. During a preoperative talk, home exercises, living rules and policies regarding physical therapy are discussed. Set goals and an end goal for yourself. It is wise to make arrangements with your employer about reintegration.
It is important to be aware of living arrangements and expectations after surgery. Ask your physical therapist or doctor about the for your specific situation.
Consider the following:
- What are the precepts?
- What exercises should you do?
- What symptoms should you look out for?
- How do you walk with crutches?
But also practical matters such as:
- How long can you not work?
- When can you ride your bike outside again?
- When will you be allowed to drive again?
- What sports can you do again soon?
Arrange your crutches in advance for after surgery. Borrowing, renting or buying from a health care storeis possible.
Keyhole knee surgery: meniscus surgery and treatment
During keyhole knee surgery, the doctor has two options for treating the meniscus.
- Meniscectomy (cutting a piece of meniscus)
- Meniscopexy (meniscus suturing)
The doctor will discuss with you which surgical technique you are eligible for.
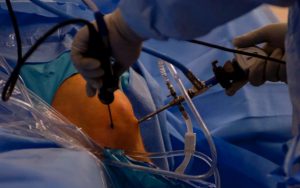
Keyhole knee surgery
Meniscectomy (wegknippen)
Rehabilitation varies from person to person and depends in part on your goals and the status of your knee preoperatively. On average, recovery takes six to 12 weeks.
After surgery, you may go home the same day. At the hospital, you will be given a protocol for your first exercises at home. The stitches will be removed after two weeks. In the first ten days you can shower with water-sealing plasters or a bag. For proper healing, the wound edges should not get too wet or soaked.
After surgery, begin stretching and bending the knee slowly. A 90-degree flexion is sufficient in the first few days. The focus is on full extension. Full extension should be achieved as soon as possible after surgery. A pillow or towel in the hollow of the knee is the biggest culprit because with this you develop a stretch limitation. Therefore, do not do it!
The load with walking and standing may be built up based on the knee's response. Increasing swelling, stiffness and/or pain are signs that you are doing too much. Tuning the load properly is important to build up the muscles. Increasing or persistent swelling causes muscle strength to decrease.
The use of crutches is usually phased out a week after surgery. Here it is important to monitor the knee's reaction. Phase out walking with crutches in consultation with your physical therapist. The exceptions are a meniscus suture and a treated cartilage defect.
Swelling in the knee disrupts muscle control and leads to decreased stability and coordinative movement. As a result, the size of the upper leg decreases. This process cannot be stopped, but can be slowed by beginning exercise immediately after surgery. The exercises focus on improving control of the thigh muscles and cooperation between them. At first, the knee does not like pressure (standing and walking) but does like unloaded movement. For this reason, it is important to do a lot of bending and stretching exercises. Once the knee can be bent 100 degrees, cycling on the exercise bike is possible. Cycling is medicine for the knee. No pressure on the knee and still a lot of exercise in a relatively short time. Cycling may be done, after consulting with your physical therapist, two to three times a day for half an hour.
Once the fluid decreases and the extension and flexion recover, training can be built up. Training consists of strength training, functional exercises and stability and coordination. However, training does not stop at training the leg muscles. A strong knee starts with a trained core, abdominal and back muscles. This becomes more important when the desire is to return to sports. A specialized sports physical therapist can guide you through this.
After two weeks, you can resume most activities of daily living.
On average, the knee is recovered after six weeks and sports can be resumed under the supervision of the physical therapist. After three to six months, you can fully resume your sport.
After one to two weeks, if the knee feels reliable, you may return to driving and bicycling (consult with your physical therapist). About 80 percent of people are back to work after two weeks. How long it takes for you depends on your recovery and type of work (heavier physical work takes longer).
Tips:
- If you have a sedentary job, try to change positions and move the knee regularly. Do your exercises to keep the knee from stiffening up.
- While sleeping, place a pillow between the knees.
- The knee may flex after surgery, but keep in mind the wounds need to recover first. Stretching is most important!
- It may take several months until squatting and kneeling is possible again.
- Swelling can remain present for six, eight and sometimes longer.
- Cooling with ice is pleasant and effective against pain.
Meniscopexy (meniscus suturing)
After surgery, you may go home on the same day. With the suture, the edges of the meniscus tear are placed back together. This allows the meniscus to recover. The suture must be protected. You may not load the knee 100 percent yet, and there is a limitation with the amount of bending. Crutches are needed to reduce the load on the knee, and sometimes a knee brace is helpful to protect the knee.
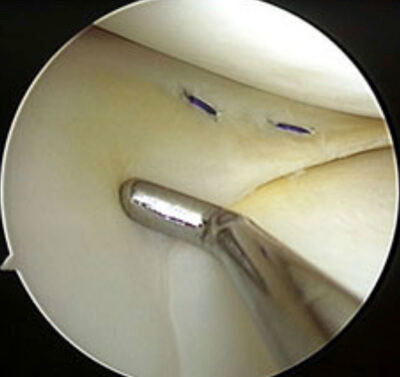
Meniscopexie (meniscushechting)
Living rules after meniscopexy:
- Do not bend the knee beyond 90 degrees for 6 weeks after surgery.
- Use crutches so that the knee can be loaded 50 percent for 6 weeks after surgery.
- Avoid deep squatting for 3 months after surgery.
- Avoid rotations for 3 months after surgery.
The living rules and protecting the suture are the biggest difference between cutting away and suturing the meniscus. Because of this, rehabilitation automatically takes longer and is more intensive. This must be taken into account in some situations (top sports/work).
Rehabilitation lasts from 3 to 6 months. It takes place under the supervision of a specialized physical therapist. The operated leg loses a lot of strength and stability in the first 6 weeks. During this phase, exercises will be done within the limitations to maintain as much of the coordination, strength and stability as possible. In this way you will be well prepared to walk without crutches after 6 weeks, be able to ride a bike again and perform other movements. The training will be gradually intensified. Ultimately, the rehabilitation focuses on your specific goals and sport.
Results of keyhole surgery of the knee
Meniscectomie:
A distinction must be made between an acute meniscus injury and a degenerative meniscus tear. An acute meniscus injury generally recovers well after surgery. In the longer term, however, the risk of osteoarthritis increases. With a degenerative meniscus tear, the short- and long-term effects of surgery are little different from conservative treatment.
Conservative treatment has a positive effect in a degenerative meniscus tear.
- After three months, 60 percent can move better.
- After six to 12 months, 64 percent move better.
- Less pain is experienced within 3 months, but the pain is generally not yet gone.
- 29 percent ended up wanting surgery anyway, but their recovery was no better than in people after conservative treatment.
- After meniscus surgery, 58 percent can move better after three months.
- After six months it is 69 percent and after a year it is 77 percent.
- Within 3 months, the pain is less, but not completely gone.
- Surgery helps as much as fake surgery.
- The risk of osteoarthritis increases over the long term.
- 80 percent of people no longer have symptoms 10 years after surgery.
In conclusion, surgery for a degenerative meniscus makes little to no difference compared to conservative treatment.
The outcome of surgical treatment of an acute meniscus injury is generally good. In the longer term, the risk of osteoarthritis increases. However, other factors such as obesity, intense athletic load or work affect the development of osteoarthritis.
Meniscopexy:
A torn cruciate ligament often accompanies a torn meniscus. If you repair the meniscus but not the cruciate ligament, the success rate is around 30 to 50 percent. An anterior cruciate ligament reconstruction should be done relatively soon (2-6 weeks) after anterior cruciate ligament surgery to give the knee adequate stability.
The success rate of a meniscopexy is 70 percent to 90 percent, and the majority of those operated on are satisfied with the result. Sports resumption is almost always possible again. The road back to full recovery varies from person to person. A knee is usually swollen a bit longer than with a meniscectomy and remains more sensitive where the suture was placed.
After three months, you can return to normal daily activities. Full flexion of the knee is usually sensitive and/or limited for some time. Sports are possible again after three to six months. The speed of return depends on the type of sport, intensity and level.
Sports with a lot of twisting and jumping (such as soccer) carry a higher risk of re-injuring the meniscus.
The risks of meniscus surgery
Degenerative meniscus:
The main risk with a degenerative meniscus tear is that you will not do better after surgery than before. Take the time to recover and work with your physical therapist to focus on the factors that are negatively affecting your recovery. Set realistic goals and adjust them if necessary should they prove unachievable. The risk of osteoarthritis increases after a meniscectomy.
With an acute meniscus tear, few risks are present other than the normal operative risks. Recovery is generally good, but may take longer due to accompanying injuries (cartilage/cross ligament).
For a degenerative and acute meniscus tear:During rehabilitation, there is a chance that the knee will stiffen, continue to hurt, wounds will be sensitive and/or bleed. A hematoma, bruise, may be visible. Usually these symptoms subside over the course of several weeks. A cutaneous nerve may be hit during surgery, causing a piece of skin in the lower leg to feel different. This is usually temporary and gradually recovers.
The knee may be irritated and swollen for long periods of time, making rehabilitation longer and difficult to build up. Muscles and tendons may also become overused during rehabilitation.
What most people suffer from is kneecap pain. It may feel like the knee is locking up and/or hurting in the front. This goes away over time, once strength recovers.
Meniscopexy:
In 10 to 30 percent of cases, the sutured meniscus does not heal properly due to inadequate adherence to the precepts, overloading the knee or twisting the knee again. As a result, there is a chance that the knee will require reoperation in which the piece of meniscus is removed.
It is normal for the knee to be swollen, stiff and painful after surgery. The stab holes are sensitive and may feel thickened. This will subside over time. The puncture holes may continue to bleed. A bruise may appear immediately and sometimes after a few days, which is normal. During surgery a cutaneous nerve may be touched, which may cause a piece of skin in the lower leg to feel different. This is usually temporary. Muscles and tendons can become overloaded during rehabilitation. It is therefore important to train with a specialized physical therapist. What most people suffer from is kneecap pain. It may feel like the knee is locking up and/or hurting in the front. This will go away over time, once strength recovers.
Again; you get one chance, stick to the precepts!
General
The surgery itself also comes with some more serious risks. You can think of:
- Wound inflammation
- Knee joint infection
- Thrombosis leg
- Pulmonary embolism
Contact the hospital immediately in the following cases:
- Increasing swelling of the knee combined with increasing pain.
- Not being able to stand on the leg when previously this was possible.
- Fever (> 38.5 degrees).
- Thick, warm, red and painful lower leg/calf.
- If you don't trust it always contact the hospital.
How much does physical therapy cost after meniscus surgery?
In the Netherlands, insurance is well regulated. Everyone has basic insurance. Still, there are usually many questions about insurance and physical therapy reimbursement.
Conservative:
With conservative rehabilitation, physical therapy is not covered by basic insurance. If you have supplementary insurance for physiotherapy, you can use this for guidance during rehabilitation. If this is not or insufficiently the case, you pay the (remaining) physiotherapy treatments yourself.
Operative:
After surgery, you usually need intensive physical therapy. The system in the Netherlands is set up so that you need 20 treatments to fall into a chronic care program. From the 21st treatment you are chronically (unlimited medically necessary) insured for one year of physiotherapy from the date of surgery. A referral from the orthopedist is necessary for this.
For the first 20 treatments, you can insure yourself through your supplementary insurance. If you have supplementary insurance for 9 treatments, you pay for 11 treatments yourself. If you don't have supplementary insurance, you pay 20 treatments yourself. One physical therapy treatment costs about 25-35 euros.
Treatment from the supplementary package is not at the expense of your deductible. Once treatments are declared from the basic package, so from 21st treatment, you do pay excess. The operation is also paid from your deductible. The deductible runs per calendar year. If the physiotherapy treatment continues after January 1, you pay your deductible again.
After reading this information about insurance and the deductible, it is quite possible that you have questions or are unclear. The situation may vary from person to person, so always consult with your physical therapist and carefully read the terms and conditions of your insurance.
