What tendon is your anterior cruciate ligament made of?

Written by Michael de Levie

Co-written by dr. Wybren van der Wal
There are four different tendons an orthopedic surgeon can choose from to restore knee stability during anterior cruciate ligament surgery. Which tendon is right for you and what the differences and similarities are between the tendons is discussed in this blog.
The differences between the hamstring tendon, patellapees. quadricepstendon and donor tendon.
Michael de Levie and Wybren van der Wal Orthopedic surgeon at hospital the Gelderse Vallei in Ede.
What is an anterior cruciate ligament?
The ACL is a Dynamic structure, rich in neurovascular supply and comprised of distinct bundles, which function synergistically to facilitate normal knee kinematics in concert with bony morphology. Characterized by individual uniqueness, the ACL is inherently subject to both anatomic and morphological variations as well as physiologic aging.
– Freddie Fu –
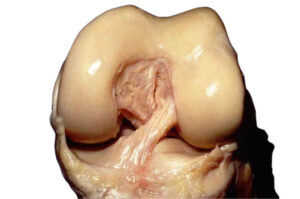
Which tendon can a doctor choose?
For a ACL surgery different types of tendons can be used. A simple division can be made between the body's own material (autograft), donor material (allograft) and synthetic material. In addition, in some cases the body's own anterior cruciate ligament sutured worden. In a first anterior cruciate ligament surgery, body-specific material (autograft) is almost always chosen. Exceptions are possible, of course.
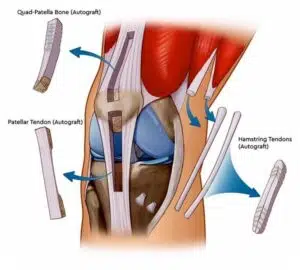
The different tendons from which an anterior cruciate ligament is made.
The anterior cruciate ligament surgery in 5 steps
- Removing the tendon from the thigh.
- Watch surgery; the knee is assessed on the inside and any other injuries are treated (such as a meniscus tear or cartilage defect)
- Drilling tunnels in the lower leg and upper leg (into which the new cruciate ligament will be placed)
- Inserting and fixing the cruciate ligament in the tunnels
- Closing the wounds.
The anterior cruciate ligament surgery by hamstring technique.
Autograft (body's own material):
The advantages of an autograft are that it is the body's own material which will not be rejected. Furthermore, the risk of retearing the reconstructed cruciate ligament is lower when using an autograft compared to an allograft (donor material). In addition, it is cheaper to use autograft material than donor material.
With an autograft, the orthopedic surgeon can choose from three tendons. The knieschijfpees (patellapees) en de hamstring tendon are the most commonly used grafts. The quadricepstendon has been increasingly used since recent years.
This person has had multiple anterior cruciate ligament surgeries.
Donor tendon
The preference is always to perform anterior cruciate ligament reconstruction with the body's own material. In exceptional cases or multiligamentous ligament injuries, the doctor may opt for a donor tendon. Want to know more about the indication for a donor tendon and what the pros and cons are click here.
History of use of plastic materials:
In the past, plastic materials were more often used to make an anterior cruciate ligament plastic. The benefits are the same as with a donor tendon, only the high recurrence rate led to this being discontinued. But developments are not standing still.
New techniques in anterior cruciate ligament surgery.
ACL repair
In recent years, there has been increasing research into repairing one's own cruciate ligament. Recently, a study was started in the Netherlands that is being conducted at several hospitals. The study examines whether the own cruciate ligament can be repaired in selected patients. It involves cruciate ligament injuries in which the cruciate ligament is torn at the location of the upper leg. The torn cruciate ligament is sutured back and reinforced with a plastic band. The great advantage is that the patient's own tissue is preserved and only narrow tunnels need to be drilled. It is also possible to return to the old level of sports faster.
There are an increasing number of studies reporting that the anterior cruciate ligament has a chance of spontaneous repair. In ons blog gaan we hier dieper op in (volgt nog). In 50-60% of cases, the anterior cruciate ligament attaches to the posterior cruciate ligament, regaining some stability. This blog discusses this. The spontaneous repair and or reattachment of the anterior cruciate ligament has led to the BEAR technique (Brigde, Enhanced ACL Repair). The cruciate ligament is sutured and given additional stimulation with its own blood to grow back into place. This procedure should be performed within three weeks. The advantage for young athletes is that this is a technique where only small drill tunnels are made. As a result, there is a lower risk of damaging the growth plates. The results have now only been carried out in pilot(s) studies (USA), but the prospects are interesting.
Take home message
Which tendon your anterior cruciate ligament is made of is helpful to know. It is good to know the pros and cons of the different grafts (hamstring, quadricepstendon, patella tendon of donor tendon). The specialist will carefully determine with you the appropriate graft choice. All in all, the results of the different graft choices are close to each other. In fact, a study is currently underway in which no difference is expected between the different grafts. Of course, an update will follow when these results are known.
However, the choice of graft is only one of many factors in the success of anterior cruciate ligament reconstruction.
Some key factors affecting recovery:
- Being selective with who qualifies for anterior cruciate ligament reconstruction.
- Surgical technique (tunnel placement)
- Other injuries such as meniscus, cartilage and/or ligament injuries
- Preparation for surgery
- Status and function of the knee before surgery
- Knee rehab
- Psychological factors
- Therapy compliance
- Going through surgery and rehabilitation at a knee specialist.
If after reading this blog "which tendon is your anterior cruciate ligament made of?" you still have questions, discuss your questions with your doctor and/or physical therapist. Optionally, you can leave a also a message and people in the network can respond or clients to share their experience.
Special thanks to: dr. Wybren van der Wal Orthopedic surgeon at the Gelderse Vallei in Ede.
Podcast: van welke pees wordt jouw voorste kruisband gemaakt? door Wybren van der Wal